My Fibre Guide
Fibre, fibre, fibre! What's all the fuss about?
I know….I keep banging on about fibre.
Eat more fibre. Add fibre to your diet. Have you tried fibre?
Over 90% of adults don’t get enough of it. Most people eat around 15g daily when they need 25-30g. That’s a big gap that’s worth closing.
So what actually is fibre? Are there different types? Why should you care?
Let’s dive in.
What is Fibre?
Fibre is the part of plants your body cannot digest.
Unlike proteins, fats, and carbohydrates (which your body breaks down and absorbs), fibre passes through your stomach and small intestine largely intact. It reaches your large intestine whole….and that’s where the magic happens.
Think of it as food for your gut bacteria. The trillions of microbes living in your colon feast on fibre, producing beneficial compounds in return.
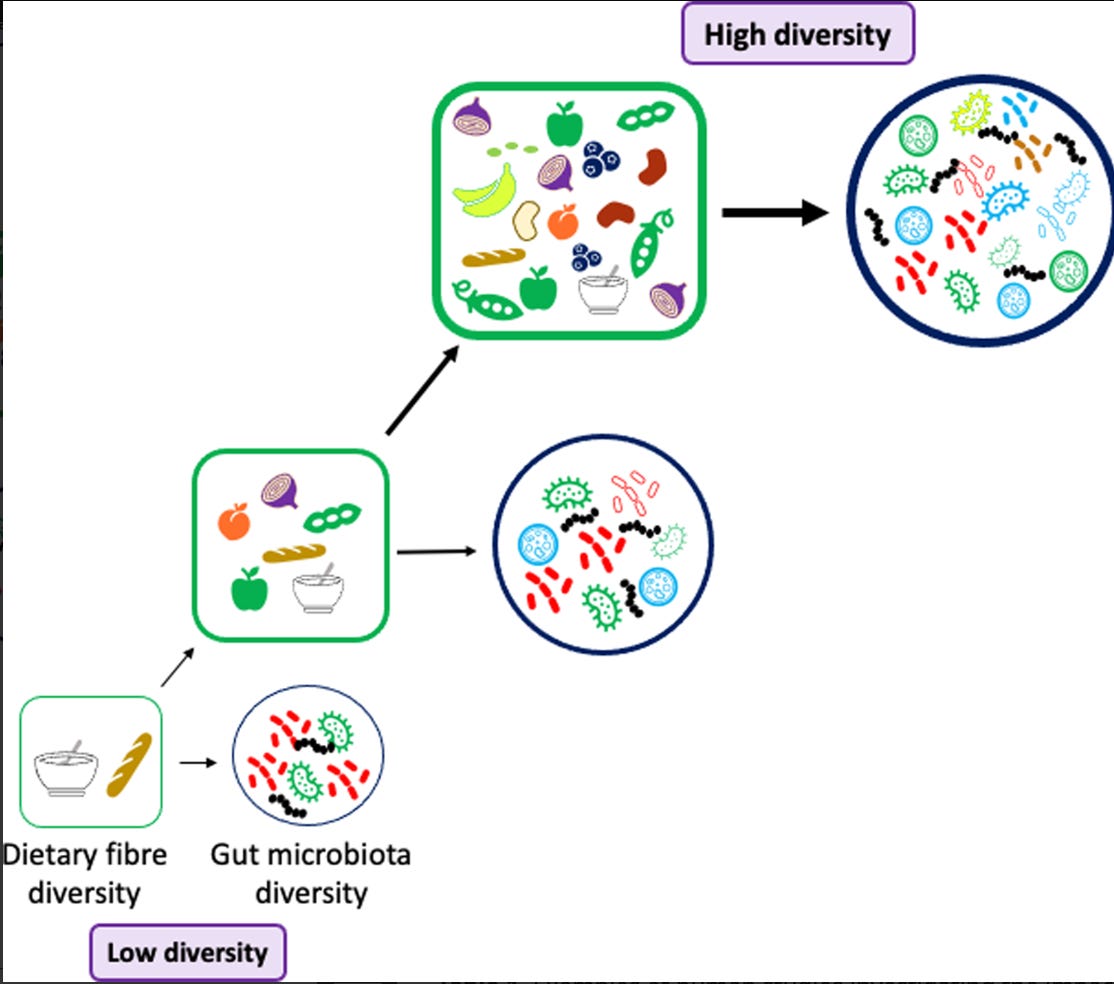
Two Types: Soluble vs Insoluble
Soluble fibre dissolves in water to form a gel-like substance. It slows digestion, helps control blood sugar, and binds to cholesterol.
Find it in oats, apples, beans, and psyllium husk (my favourite!).
Insoluble fibre doesn’t dissolve. It adds bulk to your stool and speeds things along. Find it in wheat bran, vegetables, and whole grains.
Both are helpful but work differently.
A word on bloating: Some high-fibre foods contain raffinose, a complex sugar humans can’t digest. Your gut bacteria do the job instead, producing gas in the process. Beans, cabbage, Brussels sprouts, and broccoli are the usual suspects.
This doesn’t mean avoid them. It means introduce them gradually.
Usually within 2-4 weeks, the bloating settles.]
Why Should You Eat Fibre?
Three reasons. All backed by serious evidence.
1. Stool regulation
A 2022 meta-analysis of 16 randomised controlled trials found fibre supplementation significantly improved constipation. Response rate? 66% in fibre groups versus 41% on placebo. Stool frequency increased and consistency improved.
Eat fibre = solid log 🪵
2. Gut microbiome
Your gut bacteria ferment fibre into short-chain fatty acids (SCFAs), particularly butyrate. Butyrate is the primary fuel source for your colon cells. It maintains the gut barrier, reduces inflammation, and keeps the intestinal lining healthy.
A meta-analysis of 64 RCTs showed fibre significantly increased beneficial Bifidobacterium and Lactobacillus species.
More fibre = more friendly bacteria. Another simple equation.
3. Cancer risk reduction
A landmark BMJ meta-analysis of 25 prospective studies (nearly 2 million participants) found every 10g of daily fibre reduced colorectal cancer risk by 10%. The mechanism? Faster transit time means less carcinogen exposure. Butyrate inhibits tumour cell growth. Increased stool bulk dilutes harmful compounds. The World Cancer Research Fund now rates the evidence as “convincing.”
New to Fibre? Start Slow
Going from 15g to 30g overnight is a recipe for discomfort.
Instead: increase by 2-3g every few days. Spread intake across meals. Drink plenty of water (1.5-2 litres daily). Give your gut time to adapt.
Start with gentler options: oats, cooked vegetables, psyllium. Save the beans and raw cruciferous vegetables for later, once your system has adjusted.
Patience and build it up slowwly.
Psyllium Husk: The Gold Standard
If I had to recommend one fibre supplement, it would be psyllium husk. Here’s why.
Psyllium is unique. It’s soluble, gel-forming, and (crucially) non-fermenting. Most soluble fibres get rapidly broken down by gut bacteria, producing gas. Psyllium resists this.
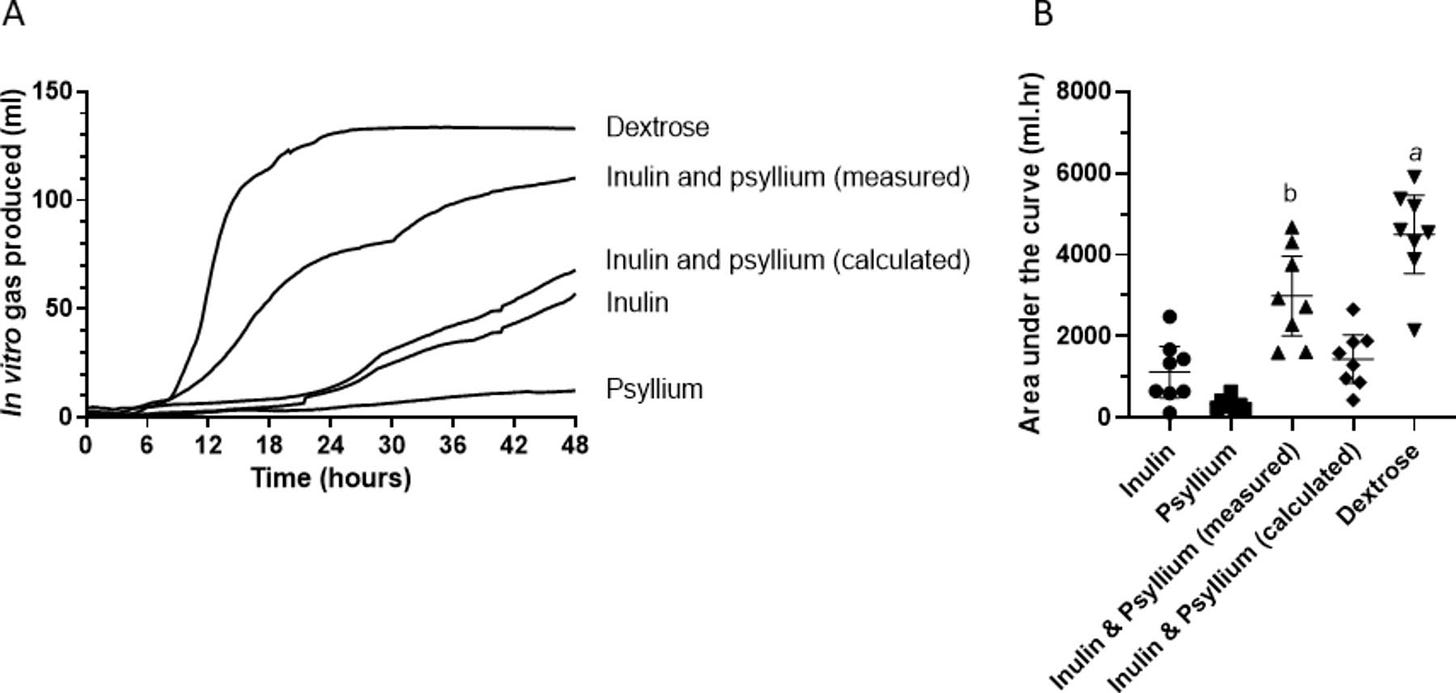
An MRI study published in Gut found psyllium caused five times less colonic gas than inulin.
Less gas, therefore Less bloating.
The evidence for bowel health is robust. A large IBS fibre trial (275 patients, published in the BMJ) compared psyllium, wheat bran, and placebo over 12 weeks. At month one, 57% of psyllium patients reported adequate relief versus 35% on placebo. Symptom severity dropped by 90 points on psyllium, compared to 49 on placebo. Wheat bran? No significant benefit over placebo. In fact, more patients dropped out of the bran group because their symptoms worsened.
The American College of Gastroenterology now recommends psyllium as the only fibre supplement with sufficient evidence for chronic constipation.
And yes, despite being non-fermenting, psyllium still supports gut bacteria. A 2019 study found it increased butyrate-producing species. Slow fermentation, it turns out, still counts.
How to take it: Mix one teaspoon (5g) of psyllium husk powder in a large glass of water (250-300ml). Stir vigorously. Drink immediately before it gels. Follow with another glass of water.
Start with half a teaspoon daily and build up over a week or two.
A simple recipe: Add one teaspoon to your morning porridge after cooking (not before, or it becomes gluey). Stir well. Top with berries and a drizzle of honey. You won’t notice it’s there….but your gut will.
Critical warning: never take psyllium without adequate liquid. It absorbs water. Without enough fluid, it can cause obstruction. Always drink plenty.
Fibre is getting the limelight….finally!
The evidence is clear. Better bowels. Healthier gut bacteria. Reduced cancer risk.
All from eating plants your body can’t digest.
Sometimes the boring solutions are the best ones.
If you enjoyed this article check out my Substack here
Struggling with liver or digestive issues that affect your daily life? Invest in your gut health with a private, personalised consultation where I will explore your specific symptoms and develop a targeted treatment plan. Take the first step toward digestive wellness today: https://bucksgastroenterology.co.uk/contact/ (I offer both in person and video consultations!)
References
1. van der Schoot A, et al. The effect of fiber supplementation on chronic constipation in adults: An updated systematic review and meta-analysis of randomized controlled trials. American Journal of Clinical Nutrition. 2022;116(4):953-969.
2. So D, et al. Dietary fiber intervention on gut microbiota composition in healthy adults: a systematic review and meta-analysis. American Journal of Clinical Nutrition. 2018;107(6):965-983.
3. Aune D, et al. Dietary fibre, whole grains, and risk of colorectal cancer: systematic review and dose-response meta-analysis of prospective studies. BMJ. 2011;343:d6617.
4. Bijkerk CJ, et al. Soluble or insoluble fibre in irritable bowel syndrome in primary care? Randomised placebo controlled trial. BMJ. 2009;339:b3154.
5. Gunn D, et al. Psyllium reduces inulin-induced colonic gas production in IBS: MRI and in vitro fermentation studies. Gut. 2022;71(5):919-927.
6. Jalanka J, et al. The Effect of Psyllium Husk on Intestinal Microbiota in Constipated Patients and Healthy Controls. International Journal of Molecular Sciences. 2019;20(2):433.
7. McRorie JW. Evidence-Based Approach to Fiber Supplements and Clinically Meaningful Health Benefits. Nutrition Today. 2015;50(2):82-89.
8. World Cancer Research Fund/AICR. Continuous Update Project: Colorectal Cancer Report. 2016.
General Disclaimer
Please note that the opinions expressed here are those of Dr Hussenbux and do not necessarily reflect the positions of Buckinghamshire Healthcare NHS Trust. The advice is intended as general and should not be interpreted as personal clinical advice. If you have problems, please tell your healthcare professional, who will be able to help you. Thank you to the amazing photographers from Unsplash where I get most of my images from.





Dr., Thank you yet again for such great info. And the helpful graph! Question for you: Do you yourself drink or eat psyllium husks daily? I have for long periods of time (when I was having stomach problems as I used to suffer from diverticulitis and only occasionally get flare ups now) so I'm not consistent with psyllium but wondering your opinion....if you think it's a necessary supplement for anyone like myself who does have a lot of soluble and insoluble fiber in my diet.
Why not add one more thing to my morning oatmeal? So far I’ve added hemp hearts and ground flaxseed, plus blueberries. It’s a hearty breakfast!